Employing the MSAM in Attaining, Maintaining and Transferring Fluency in the Schools
 |
About the presenter: Kay M. Monkhouse is the Founder of the Stuttering Institute of Princeton. She obtained her Diploma of Speech Therapy at the University of Queensland, Australia, and her BA, MA and PhD at the University of Iowa where she studied with Dean Williams. Dr. Monkhouse, who has specialized in stuttering for 20 years is currently a provider for the Speech Easy and is a certified provider for the Lidcombe Program. She is an active member of the SID 4 Stuttering Leadership Conference and served on the inaugural Malcolm Fraser Award Committee. She is one of the initial cadre of Stuttering Specialists and is a Mentor for the BRSFD. |
Employing the MSAM in Attaining, Maintaining and Transferring Fluency in the Schools
by Kay Monkhouse
from Pennsylvania, USA
Abstract
The purpose of this paper is to provide clinicians with a practical model for working with clients who stutter. The model is used to assist in counseling client, family members, teachers and other professional colleagues in establishing appropriate expectation levels for the sequence and rate of clinical progress within an increasingly complex hierarchy of environmental contexts.
The Monkhouse Skill Acquisition Model (MSAM) has been a successful clinical tool for the treatment of fluency disorders in a Private Practice setting for many years. It consists of a 4x4 matrix in which four sequential steps of skill acquisition interact with four increasingly difficult environmental complexity levels. A client must therefore negotiate all sixteen stages of the model to achieve a particular communication skill at the spontaneous level in the outside world. Because all team members complete a matrix on a regular basis, frustration is kept at a minimum (for both client and team members such as parents and teachers) since everyone involved knows the expectation level of that particular stage.
Other positive results from using the pragmatic model include (a) increased enthusiasm for attending sessions and completing home assignments, (b) an improvement in observational skills, (c) an increase in the clients' sense of direction and responsibility toward their own goals, (d) an improvement in clinician accountability and (e) it can be used with a wide age-range. A major benefit is that the model is non-categorical, and is applicable across all long-term and short-term fluency goals.
Summary
Not only is generalization (carry-over of a desired speech/language behavior into the outside world) one of the most difficult goals of therapy to achieve, it is also a perplexing concept for parents, teachers and other professionals to understand. When a client is able to achieve behavior change in communication skills during a treatment session, disappointment is frequently expressed when the observer (teacher/parent/spouse or even the client himself) does not begin to hear the newly acquired skill at home/school/in the outside world as quickly as expected. Even though we explain that changes in speaking behavior are complex, and that they occur in a sequential order, the listener appears to need more specific information about the components of this sequence, and when they will occur in the therapeutic process. Scores on tests are received with polite equanimity. The burning question that is most relevant to these listeners is not what is changing, but when will it be fixed?
Purpose
The purpose of this paper is to present a clinical model for understanding the stages in the process of skill acquisition. The success of the model appears to lie in its power to establish appropriate expectation levels for clients, family members, teachers and other professional colleagues in (a) understanding the process of achieving therapeutic goals for improved fluency skills and (b) evaluating clinical progress pragmatically. We have found that by providing a visual perspective for treatment goals and achievements, that the "listeners" in a client's various communication environments become more realistic (and therefore more positive) about therapeutic goals and the rate of clinical progress.
The basic model and terminology were first presented to this clinician in a laboratory course on "Skills for Calling and Caring Ministries - Learning the Language of Healing", developed by Kenneth J. Mitchell and John S. Savage of LEAD Consultants, Pittsford, New York, 1979.
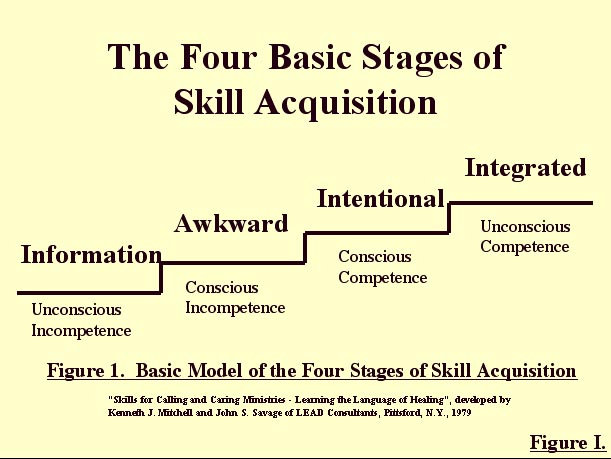
According to Mitchell and Savage, development of any skill involves working through four stages (see Figure I): (a) Information Gathering; (b) Awkwardness; (c) Intentionality, and (d) Integration. At the stage of Information Gathering, the new learner's skill level is depicted as "unconscious and incompetent"; at the Awkward stage as "conscious and incompetent"; at the Intentionality stage as "conscious and competent", and at the Integration stage as "unconscious and competent".
In order to take into account the ultimate goal of any treatment program - i.e., spontaneous, fluent, intelligible speech in any environment - it became obvious that in the realm of speech-language pathology, the basic model was not able to reflect the higher degrees of awkwardness, intentionality or integration of newly learned skills anticipated in environments beyond the clinic. By elaborating on the basic Mitchell and Savage model, we developed a pragmatic model of communication skill acquisition that consists of a 4x4 matrix in which there are not only the four sequential stages of skill acquisition, but also communication milieu at four different levels of increasing environmental complexity (clinic, home, school, world). (see Figure II)
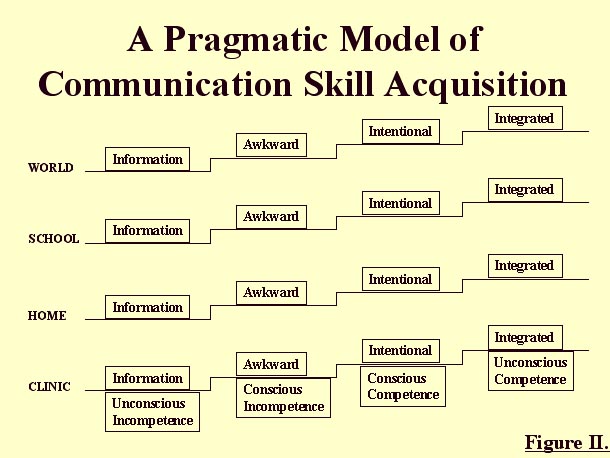
A client must negotiate all 16 stages before a "new" communication skill is spontaneous in the outside world. It is assumed that the client will be at different "stages" along the continuum for each level of complexity, but will no doubt be more advanced in the clinical setting than in any of the other three levels for a majority of the time, particularly in the early and middle stages of treatment.
The MSAM (refer to Figure III below) demonstrates the building of a hierarchy of skill acquisition in increasingly complex communication environments.
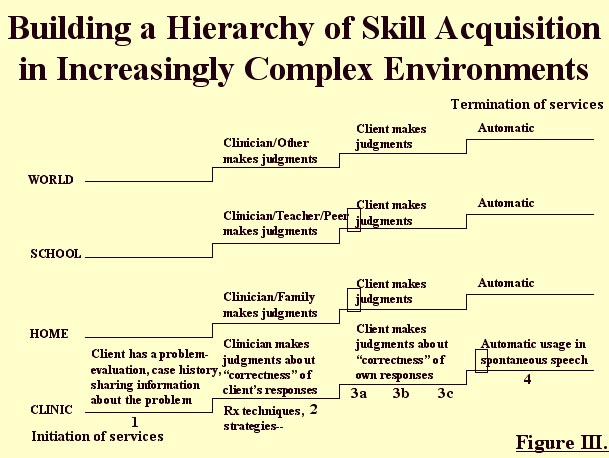
Its Mode of Use is reflected in the following stages of skill acquisition:
As treatment begins, the clinician provides a visual aid to explain expectation levels of anticipated progress, by sharing with the client and parent (and other members of the therapeutic team) the four basic steps necessary to achieve success in treatment in the clinical setting:
Stage 1: unconscious incompetence - the client doesn't know what s/he doesn't know or s/he would have fixed it. The client is a "naive recipient" of information. This is the stage where, after the case history has been taken, the evaluation completed and the diagnosis made, that the speech-language pathologist begins to convey information about the disorder and help the client isolate the particular speech behaviors that interfere with communication. Savage refers to the learner, at this stage, as being on a level of "unconscious incompetence." (The learner is not conscious - i.e., s/he is not aware of what the isolated behaviors are that contribute to the disorder and is therefore not competent in being able to make changes in those behaviors himself.) At Stage 1, therefore, the speech-language pathologist performs a formal evaluation of the client condition, informs the client/parent of the diagnosis and goals are established.
Stage 2: conscious incompetence - With ongoing treatment, with the clinician as "coach", the client begins to identify behaviors which contribute to the problem, but is at the level which Savage describes as "conscious incompetence". The learner is beginning to be aware of required behaviors and can make changes, but is not competent in being able to apply them without frequent clinician intervention. As treatment progresses, the client becomes aware of what s/he didn't know before treatment began; the clinician makes accuracy judgments
Stage 3: conscious competence - The client is conscious of the changes that need to be made and begins to make accuracy judgments about what s/he has just learned in Stage 2. As our experience with the model grew, we found it necessary to divide Stage 3 into three discrete components (3a, 3b and 3c) in order to better explain (and develop an appreciation for) the intricacies of the conscious behavior changes involved in new skill acquisition.
3b: the pre hoc "Plan." When the client has reached a stage of self-correction, s/he then moves to a competency level that allows conscious monitoring to occur ahead of time. We hear statements such as the following: "I'm not going to make that mistake again; If I'm vigilant I'll do it right the first time (even if it feels weird); I guess it has to feel wrong to be right, and, I need to force change to make it happen." The new behaviors, requiring new "muscle memory," feel very awkward and staged, and at this step, it is often necessary to remind the client that if it doesn't feel strange or uncomfortable or forced, then it is not the new way.
3c: the post hoc "Aha." This is the component of Stage 3 where the client notices after the fact that the utterance was successful. We hear statements such as the following: "Hey! Did you hear what I just did?" and "Let me tell you what I did this week!" This is a stage of self-congratulation after-the-fact, and is not only spontaneous, but is also unsolicited information, completely independent of clinician cueing or request.
Stage 4: unconscious competence - The client is reminded of our clinic motto: "If I can do it once, I can do it 1,000 times; if I can do it 4,000 times, it's a new habit!"
This pattern is then repeated at school, where either a teacher, aide or peer assumes the role of coach.
The ultimate goal is for the client to carry over the self-judgment into the outside world and thus through self-awareness, becomes his own coach.
As the sixteen steps are eventually accomplished, the client reaches a level of conscious competence in the outside world. The members of the therapeutic team are all aware of the increasing hierarchy of complexity through which the client must pass, and there is, therefore, no regression terminology, only increasing levels of complexity to explain variations/fluctuations in fluency.
Other visual aids incorporated in the treatment protocol include the Learning Curve, and the Three-Sided Coin. (see figures 4 and 5)
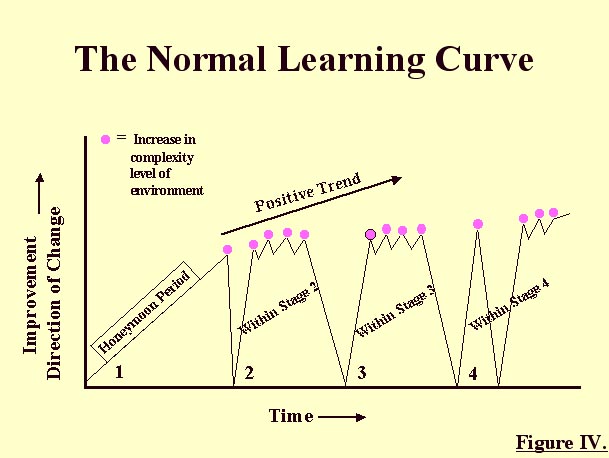

The clinician illustrates each of these as s/he explains the model and may also include the concept of a 10 point Severity Scale.
The success of this model as a clinical tool has been in its simplicity. When each member of the team is able to make a personal judgment of the client's position on the matrix, many positive results ensue. The positive pragmatic effects have been to:
- reduce anxiety and frustration for both client and listeners by establishing appropriate expectation levels (especially with multiple problems). "Listeners" become more realistic about the hierarchy of therapeutic goals and rate of clinical progress.
- Increase client's own sense of direction and responsibility towards his own goals and their attainment, and, therefore
- Increase client's enthusiasm for attending sessions and doing home assignments (particularly important for long-term treatment plans)
- Improve client's observation skills - as s/he evaluates his/her performance s/he gains confidence in negotiating his position on the continuum with other team members.
Additional side benefits have been the following:
- flexibility of the model (each step may be divided into one, two, or twenty or more subsections for psychological scaling techniques)
- improved methods of accountability (particularly in a private practice when the client or his family is paying out of pocket.)
- the model has been shown to be non-categorical (i.e., it is applicable across all communication disorders - voice, articulation and language, as well as fluency)
- the model can be understood by young children .
The MSAM thus provides a simple, positive visual tool for attaining, maintaining and transferring fluency skills, and has been particularly helpful for the therapeutic team in a school setting.
submitted September 15, 2004

