Early Identification of Stuttering Risk Level: A Brazilian Protocol Proposal
About the presenter: Claudia Regina Furquim de Andrade. Associate Professor of S�o Paulo University. Medical School. Department of Physiotherapy, Communication Science and Disorders, Occupational Therapy. Coordinator of Fluency and Fluency Disorders Laboratory. More than 70 papers and books published about prevention in speech-language disorders and fluency disorders.
Early Identification of Stuttering Risk Level: A Brazilian Protocol Proposal
by Claudia Regina Furquim de Andrade
from Brazil
This risk protocol is part of the book "Diagnóstico e Intervenção Precoce nas Gagueiras Infantis" (Stuttering in children: early intervention). It is already being used in Brazil with excellent results. The Investigation Laboratory of Fluency and Fluency Disorders has received SLP and given training for the application of the protocol. This is the experience we would like to share with our ISAD Conference colleagues in this year of 2000.
Andrade, C. R. F.de (1999). Diagnóstico e intervenção precoce nas gagueiras infantis (Stuttering in children: early intervention. São Paulo: Ed. Pró-Fono.
Abstract:
This paper proposes the application of a screening protocol for the identification of the stuttering risk level in children; from its’ onset to its’ development into chronic disfluency. This protocol is based on recent studies about risk factors which may lead to the onset and development of stuttering during childhood.
Summary:
The concept of stuttering in children is extremely controversial. As pointed by Yairi and Ambrose (1992) although it is difficult to determine exactly how and when disfluencies appear, the disorder is only noticed when certain changes in the child’s speech are considered to be a problem. Speech is marked by hesitations, repetitions, stops and other interruptions, followed or not by physical effort.
For children, as pointed by Zebrowski (1995), during the years of language development and acquisition, the existence of fluctuations in speech fluency is normal. This variation results from syntactic and semantic uncertainties and from the neuromotor maturation for speech queues. Most children surpass this period with success - almost 75% of the children recover the fluent speech pattern in 6 to 8 months after the beginning of repetitions. For the other group, disfluency remains or aggravates being followed or not by body movements. This group has a high probability of becoming chronic (Curlee and Yairi, 1997). Recognizing these children at an early stage will increase the chances of intercepting the disease’s evolutive process.
Although precise epidemiological studies on stuttering do not exist, a few authors like Yairi (1997); Curlee and Yairi (1997), Gregory (1984), Perkins (1992), Rustin and Purser (1991) bring relevant points such as: incidence is of 4 to 5% for the overall population and prevalence is of 1%. The disorder is found in the majority of cultures and natural languages; it is more frequent in males (3.5/1); a high index of spontaneous recovery exists, especially during childhood; 20 to 30% of disfluent children become stutterers; its’ distribution per age of onset is of 27% until 3 years, 68% until 3 to 7 years and 5% above 7 years.
As pointed by Smith (1990) and Craig (1994), the available evidence about the nature of stuttering suggest that it is a pathology deriving form a neuromotor deficit, which in turn creates a psychological response and has an impact on social adjustment. Although an agreement about stuttering etiological factors does not exist, certain interrelated predisponents - heredity, biological, psychological, linguistic and social factors - answer for the development of the disorder.
About heredity, based on researches and studies of Andrews and Harris (1964), Kidd (1983), Cox, Seider and Kidd (1984), Poulos and Webster (1991), Yairi and Ambrose (1992), it is known that family predisposition cannot be disregarded as a precipitant factor for the disease.
The nature of the relationship between fluency, stuttering and language formulation has been the focus of attention of several researchers (Throneburg et al., 1994; Ratner, 1995; Stager and Ludlow, 1993; Louko, 1995; Hill, 1995). In a linguistic context, elements which have large impact on speech fluency are: deficits in articulation and/or phonology acquisition and/or development; deficits in language acquisition and/or development, in terms of extension and complexity, overall syntatic-semantic-pragmatic aspects; learning difficulties, specially in reading acquisition and/or development; increased articulatory pressure; increased speech rate.
One of the greatest paradigms involving the study of stuttering is the influence of the environment, in particular the behavior and attitudes, linguistic and paralinguistic, of parents and other speakers (teachers, friends, etc) who are close to the child. The importance of family interactions, as a fundamental factor for the onset and development of stuttering , has been largely defended since the 40’s with the studies of Johnson, and is still studied until the present day (Kelly and Conture, 1992; Onslow et al., 1992; Zebrowski and Conture, 1989; Botterill et al., 1991; Conture and Kelly, 1991).
For the planning of an efficient early intervention program (Curlee and Yairi, 1997; Zebrowski, 1997; Ratner, 1997; Hill, 1997; Andrade, 1997 a/b), compromised elements of every area and how they interrelate should be investigated, selecting which are more relevant and verifying how the development in terms of severity occurs. Basic elements to be taken into consideration are: age, sex, disfluency type, time of onset, type of onset, related communicative factors, related qualitative factors, psychological factors, morbid pre-peri-post natal background, family background and the reaction of family members, the child itself and environment towards disfluency.
The protocol is composed by 15 questions and should be used with the child´s parents or guardians. After all the questions have been answered, each column has their points added, giving the therapist an idea of the child´s condition.
The screening
Screenings are by definition simple procedures; easy to use; low in cost and have a good discriminating response. The aim of a speech and language screening is to detect a communication disorder in it’s early stages. The early detection of a speech and language disorder will in turn allow the use of procedures which will make treatment most effective (Andrade, 1996). It is important to have in mind that screening by itself will not bring any benefits to health. It is an act of prevention that simply identifies who has certain risk conditions to develop a disorder or who will benefit from immediate treatment.
The concept of risk, as pointed by Ayres (1997), implies in the delimitation of susceptibility, attributable to an individual or to a group in the population, determined by the exposure to specific agents (aggressors or protectors). To determine what is considered to be of risk depends on the already established knowledge about the natural history and distribution among the population of a certain disorder. Therefore, the first point to be taken into consideration in this process is that data obtained in screenings and speech and language assessments are clearly insufficient for the early detection of risk to develop chronic stuttering.
In this way, with the use of the proposed protocol - incorporated to everyday speech and language assessment material or adapted for screenings in the population - the speech pathologist will be equipped to proceed safely in the intervention of stuttering. The obtained results will allow the identification of the child’s risk level to develop stuttering and will help in the selection of the most appropriate treatment according to each case.
STUTTERING RISK PROTOCOL
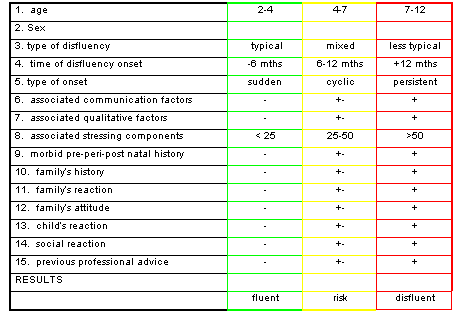
PROCEDURE
The filling in of the protocol must follow the sequence shown above, marking the correspondent column with the number o points discriminated below. After completing the questionnaire, the points corresponding to each column must be added, identifying the area with more points.
- identify in which age group the child is, put 1 point in the corresponding column
- if it’s a girl give 1 point, if it’s a boy give 2 points, put the points in the corresponding age column
- recognize which disfluency categories are present by asking the person who is being interviewed to show the type of disfluency the child usually shows. Put 1 point in the column that best describes the disfluencies shown by the child. Typical disfluencies ( hesitations, interjections, revisions, unfinished words, phrase repetitions ). Mixed disfluencies ( 1 or at the most 2 sound or syllable or word repetition, with no qualitative characteristics ). Less typical disfluencies ( 3 or more sound and/or syllable and/or word repetitions, prolongations, blocks, pauses ).
Hesitation: silent pause of one to two seconds of duration where the child seems to be looking for a word.
Interjection: inclusion of meaningless words or phrases irrelevant to the conveyed message ( well, uh, um, you know, like ).
Revision: a change in content of the conveyed message, grammatical form or pronunciation of a word ( can he she come over ? he tooked took it to the teacher ).
Unfinished word: a word which is abandoned, not completed later in the current unrevised message. Unfinished words are typically followed by revisions ( Sally wants choc vanilla ice-cream ), on occasion, the conveyed message is continued without being revised ( We went to Flori for vacation ).
Phrase repetition: the repetition of at least two complete words of the conveyed message ( It’s a beautiful a beautiful day ).
Word repetition: the repetition of a whole word including single syllable words ( What time time is it? I need a a pen ).
Syllable repetition: more than a sound repetition and less than a word repetition. Any part word repetition is included ( I want the ba ba banana. The ambulance lance passed us ).
Sound repetition: repetition of a phoneme or an element of a diphthong that does not stand alone as a word ( Do you want s s s some coffee ? ).
Prolongation: inappropriate duration of a phoneme or an element of a diphthong which may or may not be accompanied by qualitative characteristics such as pitch change, increased audible tension or visible tension ( Th_____ at’s mine. Can I have a_____ piece of cake? ).
Block: inappropriate timing in the initiation of any phoneme or the release of a stop element, usually accompanied by increased audible tension, visible tension or fixed articulatory posture ( mouth open before speaking or facial tremors before speaking etc. ).
Pause: inappropriate pause, interrupting the temporal sequence of speech ( more than 3 seconds to connect the elements ). Can be accompanied or not by qualitative characteristics.
- put 1 point in the column that corresponds, in months, to the first time the problem was noticed
- put 1 point in the column that best describes the problem’s onset. Sudden, cyclic ( appears and disappears, sometimes it’s better sometimes it’s worse ), persistent ( since the child started speaking; symptoms are constant; is getting worse with time )
- put 1 point in the column that best describes the importance of associated worsening communication factors, taking in account the child’s age group. These are: phonologic alterations ( omissions, distortions or sound change ); oral myofunctional and neurovegetative alterations; does not show speech turn-taking; does not attend satisfactorily to orders; does not have adequate comprehension of what is asked; does not have good memory; does not know the name of things; only speak short and simple phrases; only the family understands what the child is speaking. It will be negative if non of the above is shown. If the observed alterations are expected for the age group, it means to keep alert. It will be positive if one or more of the above behaviors are identified.
- put 1 point in the column that best describes the qualitative associated factors. These are: speech rate alterations ( specially acceleration ); variations in loudness ( high/low ), altered pitch ( low/high ); associated body tension; associated facial tension; ruptures caused by alterations in breathing-speaking coordination. It will be negative if non of the above is observed, alert if only one of the factors are present and positive if more than one are identified.
- put 1 point in the corresponding column. To be investigated: up to 25 points ( death of pet, change in personal habits - sleep, eating, discipline - problems with teacher or room mates, house or school moving, vacation trip ), between 25 and 50 points ( remaking of parents, father’s loss of job, mother’s beginning to work, health problems in the family or with close relatives, mother’s pregnancy, difficulties in school, birth of brother/sister, financial difficulties ), more than 50 points ( death or divorce of parents, death or sickness in close family ).
- put 1 point in the corresponding column. To be investigated: were there serious prenatal complications; pre-maturity; had to stay in neonatal intensive care; long hospitalizations; strong infections; neurological findings ( convulsions, neuroleptic medication, etc. ) . It will be negative if non of the above is observed, alert if only one of the factors are present and positive if more than one are identified or if there damage is suspected to be present.
- put 1, 2 or 3 points in the corresponding column. No risk (1) if there is no kind of inheritance. Medium risk if the genetic component is found in the distant family ( grandparents, uncles/aunts, cousins ). High risk if the genetic component is located in the close family ( parents and brothers/sisters ) or if there are several affected family members. In the corresponding column ( alert or high risk ) give 2 points when the family predisposition is accompanied by spontaneous recovery; give 3 points when chronic family predisposition exist. When the genetic component is unknown ( adopted child and/or with unknown father ) put 2 points in the alert column.
- put 1 point in the corresponding column. Positive attitude means that parents are worried and reacting adequately towards the problem. Alert attitude means that parents are not giving the problem the deserved attention, they are looking for help because it was imposed by others ( school, doctor, psychotherapist, etc.). Negative attitude means that parents are very concerned, confused and anxious, reacting strongly to the problem.
- put 1 point in the corresponding column. This item refers to the linguistic family attitudes. These are: gives more attention to disfluency than to fluency; offers "hints and tricks" to avoid disfluencies ( think before speaking, breath, keep calm, speak slowly, etc. ); finishes the child’s sentence; hurries the child to finish his speech ( come on, speak quickly I’m in a hurry and etc. ); encourages or asks the child to speak quickly, correctly and maturely constantly; frequently corrects, criticizes or modifies phrases, the pronunciation of words or sounds presented by the child; speaks too quickly, or speaks to quickly with the child; has an accelerated way of life ( everything is for yesterday ); exhibits the child to the rest of the family and friends making him read, sing, etc.; does not respond to the child when he/she needs it, only doing it when they feel like it or can; gives more attention and over protects only when disfluencies occur. It will be positive when none of the above is found. It will be considered alert if only one of the behaviors mentioned before is found. It will be negative if more than one of these behaviors are found.
- put 1 point in the corresponding column. This item refers to the child’s attitude in relation to his/hers own problem. These is: excessive shyness, does not stand frustration; excessive anxiety; often overreacts; persistent hesitation, shyness and insecurity; irritation ( rage and gets out of control ); low self-esteem; tends to self-punishment, guilt, accidents; perfectionism; sensation of failure when competing for attention; constantly seeking attention; exaggerated dependency. It will be positive when none of the above is found. It will be considered alert if only one of the behaviors mentioned before is found. It will be negative if more than one of these behaviors are found or if a compromise in the child’s self-image as a speaker is noticed.
- put 1 point in the corresponding column. This item refers to the way friends and distant family, as well as teachers and friends at school react to the problem. It will be positive if people show concern and advise parents to look for help. It will be considered alert if only some people are concerned and others offers tips on how to deal with the problem or ignore it, etc. It will be negative if no adequate attitude is shown towards the problem, or if reaction is exaggerated.
- put 1 point in the corresponding column. It will be positive if adequate advice is given, indicating other professionals to complete the diagnose. It will be alert if unclear information is given or if parents are told to wait awhile and see what happens. It will be negative if tricks and non-scientific solutions are offered.
Criteria for selecting which therapeutic program the child will enter: add all the points in each column. The column that shows the greater number of points will correspond to the therapeutic program in which the child should take part. If by any chance there are columns with equal number of points, the child should enter in the more complex program.
Members of the Investigation Laboratory of Fluency and Fluency Disorders:
Coordinator:
Dr. Claudia Regina Furquim de Andrade
Assistants:
Fernanda Chiarion Sassi
Fabíola Juste
Collaborators:
Rosana de Souza Andrea Correa Dias
Susana Garcia Francischetti Patricia Cristina Andrade Pereira
Mara Ligia Costa Daher Picarone
Cristiane Mocco Canhetti
Heliane Campanatti Ostiz
Christian César Cândido de Oliveira
Mariel Gonçalves Resende
Fernanda Regina de Souza
Luciana Maluf Cervone
Larrissa Pannunzio Oliveira
August 22, 2000

